Abstract
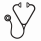
Background
Among several groups of clinicians and hematopathologists a conflict of opinion has been repeatedly expressed concerning the validity of bone marrow (BM) features characterizing myeloproliferative neoplasms (MPNs). In this regard, controversy is mainly focused on the distinction between essential thrombocythemia (ET) and pre-fibrotic/early primary myelofibrosis (pre-PMF) Although other groups confirmed the characteristic BM features and emphasized the clinical impact to discriminate both MPN subtypes the existence of pre-PMF has been questioned, including clinical usefulness and particularly reproducibility of the corresponding diagnostic guidelines. In this context, it has been criticized that the MPN classification proposed by the World Health Organization (WHO), updated in 2008 and revised in 2016,was focused on BM morphology as the gold standard of diagnosis.
The current standard for follow-up of these patients is based on pathological markers (peripheral blood counts and/ bone marrow histomorphology) and molecular markers. Bone marrow examination is the gold standard method to assess the disease's extent; it offers detailed information about cellularity, the morphology of each lineage, the degree of fibrosis, and the transformation and dysplastic features. However, many patients are reluctant to go for this invasive technique which precludes precise disease activity assessment at the desirable frequencies. A non-invasive technique that can offer reliable prognostic and predictive information about the disease is lacking.
The objective of this study is to explore the diagnostic value of FLT-PET in malignant hematopoiesis of Pre-PMF and ET. The potential to use FLT-PET metrics to differentiate between Pre-PMF and ET is assessed
Methods
A total of 13 patients (mean age of 43.23 ± 14.42 years, 7 males and 6 females) with Essential Thrombocythemia (ET) and/or Prefibrotic myelofibrosis were included in this study. One male subject was excluded due to an inconclusive diagnosis. The study was approved by the institutional review board. Written informed consents were obtained from all subjects. Each subject underwent FLT PET imaging as well as bone marrow examination (gold standard) and all were tested for JAK2v617F , CALR and MPL . Semi-quantitative (SUVmax and SUVmean) measurements of FLT uptake in the liver, spleen and Lumbar spine, SUVmean, as well as the Total Lesion Glycolysis (TLG) of the Lspine were performed. Results from the two patient cohorts were compared using = Kruskal-Wallis statistical test. A P-value of <0.05 is considered to be statistically significant.
Discussion:
Pre‐PMF and ET exhibited different features of bone marrow; however, this is not always easy to judge objectively, making pathologists' distinction often suboptimal. And in another scenario, bone marrow which is mandated for diagnosis, cannot be obtained due to technical issues or patient-related factors. In the 2016 revised classification,pre-PMF was recognized as a separate entity, distinct from ET. Thrombosis and hemorrhage represent two of the main causes of morbidity and mortality in patients with ET. Incidence of arterial and venous thrombosis prior to diagnosis revealed no significant differences (23% /20 and 9/8%) in WHO-defined ET compared with pre-PMF; thrombotic complications were also similar during the follow-thrombosis is not significantly different, whereas bleeding is more frequent in pre-PMF.From clinical prespective it is important to differentiate between the two categories.
Results
The differences in FLT SUVmax and SUVmean measurements in the three organs (liver, spleen, and LSpine) between the ET and Pre-PMF patients were not statistically significant (P>0.05). In contrast, TLG measurements in the LSpine were statistically different (P=0.013), and therefore, compared to gold standard bone marrow results, TLG can separate ET and Pre-PMF patients.
Conclusion
TLG of the Lumbar Spine in FLT PET images is a potential quantitative parameter to discriminate between ET and PRE-PMF patients
No relevant conflicts of interest to declare.
Author notes
 This icon denotes a clinically relevant abstract
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal